The Cardiac Arrest section only matters if the patient was in cardiac arrest at some point during the call. When it applies, the data here is some of the most-analyzed in EMS — your medical director, your state, and national registries like CARES all review it.
Opening the section
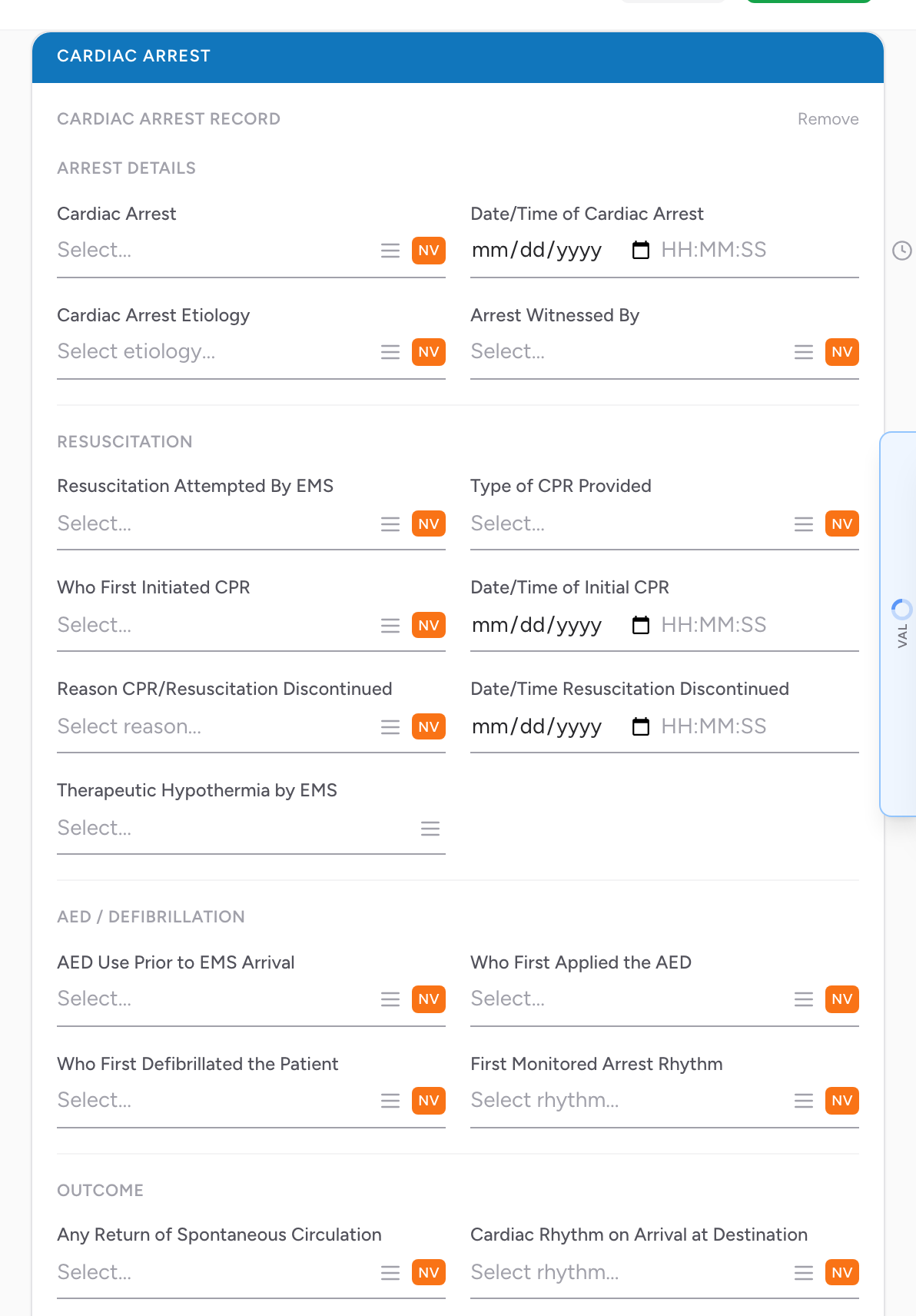
On the Assessment tab, the Cardiac Arrest section starts collapsed with a single Add Arrest button. Click it to open the section — all the fields below become visible. If the call is not a cardiac arrest, leave it collapsed.
If you open it by mistake, click Remove at the top of the section to collapse it again.
Arrest Details
- Cardiac Arrest — pick from the list whether the patient was in arrest.
- Date/Time of Cardiac Arrest — when the arrest happened. If you do not know, use the NV or PN buttons — PN has Unable to Complete and Approximate.
- Cardiac Arrest Etiology — the presumed cause (presumed cardiac, trauma, respiratory, drug, electrocution, drowning, etc.).
- Arrest Witnessed By — multi-select. Check every category that applies (family, bystander, EMS, healthcare provider).
Resuscitation
- Resuscitation Attempted By EMS — multi-select. What you did (chest compressions, defibrillation, ventilation, medication).
- Type of CPR Provided — multi-select (compressions only, compressions + ventilation, mechanical, etc.).
- Who First Initiated CPR — family, bystander, healthcare provider, first responder, EMS.
- Date/Time of Initial CPR — when CPR started.
- Reason CPR/Resuscitation Discontinued — ROSC, DNR presented, obvious death, medical control direction, time elapsed.
- Date/Time Resuscitation Discontinued — when it stopped.
- Therapeutic Hypothermia by EMS — yes / no / contraindicated.
AED / Defibrillation
- AED Use Prior to EMS Arrival — applied and shock delivered, applied no shock, not applied, unknown.
- Who First Applied the AED.
- Who First Defibrillated the Patient.
- First Monitored Arrest Rhythm — the rhythm you saw when you first got the monitor on (VF, VT, asystole, PEA, other).
Outcome
- Any Return of Spontaneous Circulation — multi-select. Check every ROSC you got (in field, during transport, on arrival).
- Cardiac Rhythm on Arrival at Destination — multi-select.
- End of EMS Cardiac Arrest Event — how the call ended for your unit (sustained ROSC to hospital, died in field, terminated, transferred).
- Neurological Outcome at Hospital Discharge — fill in if your agency follows up and you know the outcome. Most crews leave this blank; your medical director or QA team fills it in after the fact.
An example
You respond to an unresponsive patient. The husband was doing CPR when you walked in — he saw her collapse 4 minutes ago. You put her on the monitor and find ventricular fibrillation. You shock once, continue CPR, and after 6 minutes of work you get a pulse back. You transport her with a sustained pulse to a STEMI center.
Click Add Arrest. Under Arrest Details pick the value that means the patient was in arrest, enter the arrest time, etiology Presumed Cardiac, witnessed by Family. Under Resuscitation attempted Compressions, Ventilation, Defibrillation, CPR type Compressions + Ventilation, who first initiated CPR Family. Under AED / Defibrillation AED prior to EMS Not Applied, first monitored rhythm Ventricular Fibrillation. Under Outcome ROSC In Field, end of event Sustained ROSC to Hospital.
Tip: These fields feed CARES, ROC, and your state's cardiac arrest registry. Get them right the first time — registry data is almost never corrected after the fact.
